The Primary Causes And Treatment Plans Of Achilles Tendonitis
Overview
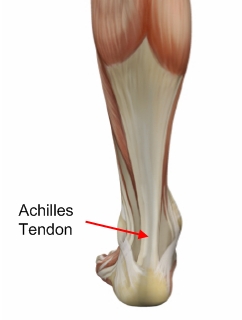 Achilles tendinitis is an overuse injury common in many sports that require lots of running and jumping. Once this condition becomes more chronic adhesions that form along the tissues and the injury becomes more of a tendinosis. Treatment for a tendinosis is much different that for a tendinitis, so it is important to recognize what stage the injury is at in order to treat it appropriately. An acute achilles tendinitis involves inflammation and would be treated with rest, ice, etc. Once the inflammation has decreased, research shows that eccentric exercises are beneficial. Once there is tendinosis, it becomes imperative to break up those adhesions with ART and prescribe appropriate stretches and exercises.
Achilles tendinitis is an overuse injury common in many sports that require lots of running and jumping. Once this condition becomes more chronic adhesions that form along the tissues and the injury becomes more of a tendinosis. Treatment for a tendinosis is much different that for a tendinitis, so it is important to recognize what stage the injury is at in order to treat it appropriately. An acute achilles tendinitis involves inflammation and would be treated with rest, ice, etc. Once the inflammation has decreased, research shows that eccentric exercises are beneficial. Once there is tendinosis, it becomes imperative to break up those adhesions with ART and prescribe appropriate stretches and exercises.
Causes
Tendinitis most often occurs when a tendon is over used. As the foot extends the Achilles tendon engages the calf muscles. The calf muscle generates force, which is transferred to the foot via this tendon. As this action repeats the tendon will endure large amounts of stress. An under-trained or inexperienced athlete is most likely to be affected by tendinitis since their body is not accustomed to the stress involved with athletics. Improper foot mechanics is another common cause of Achilles tendinitis. A properly functioning foot will distribute weight evenly across the foot. On the contrary, if the foot is experiencing improper mechanics, the weight of the body will not be evenly distributed. This can result in tendinitis, plantar fasciitis, calluses, bunions, neuromas and much more.
Symptoms
The symptoms associated with Achilles tendonitis and tendonosis include, Pain-aching, stiffness, soreness, or tenderness-within the tendon. This may occur anywhere along the tendon?s path, beginning with the tendon?s attachment directly above the heel upward to the region just below the calf muscle. Often pain appears upon arising in the morning or after periods of rest, then improves somewhat with motion but later worsens with increased activity. Tenderness, or sometimes intense pain, when the sides of the tendon are squeezed. There is less tenderness, however, when pressing directly on the back of the tendon. When the disorder progresses to degeneration, the tendon may become enlarged and may develop nodules in the area where the tissue is damaged.
Diagnosis
The diagnosis is made via discussion with your doctor and physical examination. Typically, imaging studies are not needed to make the diagnosis. However, in some cases, an ultrasound is useful in looking for evidence of degenerative changes in the tendon and to rule out tendon rupture. An MRI can be used for similar purposes, as well. Your physician will determine whether or not further studies are necessary.
Nonsurgical Treatment
In addition to stretching, using a foam roller and getting regular massage to keep the joint mobile can help prevent any problems from starting. If you start to feel inflammation in your tendon or have Achilles tendinitis once, it isn?t necessarily the end of the world. Let it rest and recover, which can sometimes take as long as four to six weeks if you waited until the pain was acute. The real problem is if Achilles tendinitis becomes an ongoing injury. If it keeps recurring, then it?s time for the perpetually injured to examine what they?re doing to cause the problem.

Surgical Treatment
Percutaneous Achilles Tendon Surgery. During this procedure the surgeon will make 3 to 4 incisions (approx. 2.5 cm long) on both sides of the Achilles tendon. Small forceps are used to free the tendon sheath (the soft tissue casing around your Achilles tendon) to make room for the surgeon to stitch/suture any tears. Skilled surgeons may perform a percutaneous achilles tendon surgery with ultrasound imaging techniques to allow for blink suturing with stab incisions made by a surgical suture needle. This procedure can be done in 3 different ways depending on the preference and experience of your surgeon. Instead of making several 2.5 cm incisions for this procedure, some surgeons will use guided imaging with an ultrasound to see the Achilles tendon tissue without having to open up your ankle. For this technique, they will use a surgical needle to repeatedly stab your Achilles tendon. These "stab incisions" will allow the surgeon to "blindly" suture your tendon without seeing the actual tissue. As another option - some surgeons will only make 1 to 3 incisions for smaller surgical implements to repair your tendon while relying on imaging ultrasound to see your damaged tissue. During either procedure the use of ultrasound imaging or endoscopic techniques requires a very skilled surgeon.
Prevention
So what are some of the things you can do to help prevent Achilles Tendinitis? Warm Up properly: A good warm up is essential in getting the body ready for any activity. A well structured warm up will prepare your heart, lungs, muscles, joints and your mind for strenuous activity. Balancing Exercises, Any activity that challenges your ability to balance, and keep your balance, will help what's called proprioception, your body's ability to know where its limbs are at any given time. Plyometric Training, Plyometric drills include jumping, skipping, bounding, and hopping type activities. These explosive types of exercises help to condition and prepare the muscles, tendons and ligaments in the lower leg and ankle joint. Footwear, Be aware of the importance of good footwear. A good pair of shoes will help to keep your ankles stable, provide adequate cushioning, and support your foot and lower leg during the running or walking motion. Cool Down properly, Just as important as warming up, a proper cool down will not only help speed recovery, but gives your body time to make the transition from exercise to rest. Rest, as most cases of Achilles tendinitis are caused by overuse, rest is probably the single biggest factor in preventing Achilles injury. Avoid over training, get plenty of rest; and prevent Achilles tendinitis.
 Achilles tendinitis is an overuse injury common in many sports that require lots of running and jumping. Once this condition becomes more chronic adhesions that form along the tissues and the injury becomes more of a tendinosis. Treatment for a tendinosis is much different that for a tendinitis, so it is important to recognize what stage the injury is at in order to treat it appropriately. An acute achilles tendinitis involves inflammation and would be treated with rest, ice, etc. Once the inflammation has decreased, research shows that eccentric exercises are beneficial. Once there is tendinosis, it becomes imperative to break up those adhesions with ART and prescribe appropriate stretches and exercises.
Achilles tendinitis is an overuse injury common in many sports that require lots of running and jumping. Once this condition becomes more chronic adhesions that form along the tissues and the injury becomes more of a tendinosis. Treatment for a tendinosis is much different that for a tendinitis, so it is important to recognize what stage the injury is at in order to treat it appropriately. An acute achilles tendinitis involves inflammation and would be treated with rest, ice, etc. Once the inflammation has decreased, research shows that eccentric exercises are beneficial. Once there is tendinosis, it becomes imperative to break up those adhesions with ART and prescribe appropriate stretches and exercises.
Causes
Tendinitis most often occurs when a tendon is over used. As the foot extends the Achilles tendon engages the calf muscles. The calf muscle generates force, which is transferred to the foot via this tendon. As this action repeats the tendon will endure large amounts of stress. An under-trained or inexperienced athlete is most likely to be affected by tendinitis since their body is not accustomed to the stress involved with athletics. Improper foot mechanics is another common cause of Achilles tendinitis. A properly functioning foot will distribute weight evenly across the foot. On the contrary, if the foot is experiencing improper mechanics, the weight of the body will not be evenly distributed. This can result in tendinitis, plantar fasciitis, calluses, bunions, neuromas and much more.
Symptoms
The symptoms associated with Achilles tendonitis and tendonosis include, Pain-aching, stiffness, soreness, or tenderness-within the tendon. This may occur anywhere along the tendon?s path, beginning with the tendon?s attachment directly above the heel upward to the region just below the calf muscle. Often pain appears upon arising in the morning or after periods of rest, then improves somewhat with motion but later worsens with increased activity. Tenderness, or sometimes intense pain, when the sides of the tendon are squeezed. There is less tenderness, however, when pressing directly on the back of the tendon. When the disorder progresses to degeneration, the tendon may become enlarged and may develop nodules in the area where the tissue is damaged.
Diagnosis
The diagnosis is made via discussion with your doctor and physical examination. Typically, imaging studies are not needed to make the diagnosis. However, in some cases, an ultrasound is useful in looking for evidence of degenerative changes in the tendon and to rule out tendon rupture. An MRI can be used for similar purposes, as well. Your physician will determine whether or not further studies are necessary.
Nonsurgical Treatment
In addition to stretching, using a foam roller and getting regular massage to keep the joint mobile can help prevent any problems from starting. If you start to feel inflammation in your tendon or have Achilles tendinitis once, it isn?t necessarily the end of the world. Let it rest and recover, which can sometimes take as long as four to six weeks if you waited until the pain was acute. The real problem is if Achilles tendinitis becomes an ongoing injury. If it keeps recurring, then it?s time for the perpetually injured to examine what they?re doing to cause the problem.

Surgical Treatment
Percutaneous Achilles Tendon Surgery. During this procedure the surgeon will make 3 to 4 incisions (approx. 2.5 cm long) on both sides of the Achilles tendon. Small forceps are used to free the tendon sheath (the soft tissue casing around your Achilles tendon) to make room for the surgeon to stitch/suture any tears. Skilled surgeons may perform a percutaneous achilles tendon surgery with ultrasound imaging techniques to allow for blink suturing with stab incisions made by a surgical suture needle. This procedure can be done in 3 different ways depending on the preference and experience of your surgeon. Instead of making several 2.5 cm incisions for this procedure, some surgeons will use guided imaging with an ultrasound to see the Achilles tendon tissue without having to open up your ankle. For this technique, they will use a surgical needle to repeatedly stab your Achilles tendon. These "stab incisions" will allow the surgeon to "blindly" suture your tendon without seeing the actual tissue. As another option - some surgeons will only make 1 to 3 incisions for smaller surgical implements to repair your tendon while relying on imaging ultrasound to see your damaged tissue. During either procedure the use of ultrasound imaging or endoscopic techniques requires a very skilled surgeon.
Prevention
So what are some of the things you can do to help prevent Achilles Tendinitis? Warm Up properly: A good warm up is essential in getting the body ready for any activity. A well structured warm up will prepare your heart, lungs, muscles, joints and your mind for strenuous activity. Balancing Exercises, Any activity that challenges your ability to balance, and keep your balance, will help what's called proprioception, your body's ability to know where its limbs are at any given time. Plyometric Training, Plyometric drills include jumping, skipping, bounding, and hopping type activities. These explosive types of exercises help to condition and prepare the muscles, tendons and ligaments in the lower leg and ankle joint. Footwear, Be aware of the importance of good footwear. A good pair of shoes will help to keep your ankles stable, provide adequate cushioning, and support your foot and lower leg during the running or walking motion. Cool Down properly, Just as important as warming up, a proper cool down will not only help speed recovery, but gives your body time to make the transition from exercise to rest. Rest, as most cases of Achilles tendinitis are caused by overuse, rest is probably the single biggest factor in preventing Achilles injury. Avoid over training, get plenty of rest; and prevent Achilles tendinitis.
Achilles Tendinitis Treatments And Causes
Overview
 The Achilles tendon connects the calf muscles in the lower leg to the heel bone. It is the largest yet most exposed tendon in the body. Achilles tendonitis is where the Achilles tendon, and sometimes the protective sheath through which it moves, becomes inflamed, causing pain and swelling symptoms. Achilles tendonitis (also known as Achilles tendinopathy or tendonosis) is classified as an overuse injury. If left untreated it can become chronic (long-term), requiring more intensive treatment. Achilles tendonitis can also increase the risk of sustaining an Achilles tendon rupture (tear).
The Achilles tendon connects the calf muscles in the lower leg to the heel bone. It is the largest yet most exposed tendon in the body. Achilles tendonitis is where the Achilles tendon, and sometimes the protective sheath through which it moves, becomes inflamed, causing pain and swelling symptoms. Achilles tendonitis (also known as Achilles tendinopathy or tendonosis) is classified as an overuse injury. If left untreated it can become chronic (long-term), requiring more intensive treatment. Achilles tendonitis can also increase the risk of sustaining an Achilles tendon rupture (tear).
Causes
Although a specific incident of overstretching can cause an Achilles tendon disorder, these injuries typically result from a gradually progressive overload of the Achilles tendon or its attachment to bone. The cause of this chronic overload is usually a combination of factors that can put excess stress on the tendon: being overweight, having a tight calf muscle, standing or walking for a long period of time, wearing excessively stiff or flat footwear, or engaging in significant sports activity.
Symptoms
Gradual onset of pain and stiffness over the tendon, which may improve with heat or walking and worsen with strenuous activity. Tenderness of the tendon on palpation. There may also be crepitus and swelling. Pain on active movement of the ankle joint. Ultrasound or MRI may be necessary to differentiate tendonitis from a partial tendon rupture.
Diagnosis
The diagnosis is made via discussion with your doctor and physical examination. Typically, imaging studies are not needed to make the diagnosis. However, in some cases, an ultrasound is useful in looking for evidence of degenerative changes in the tendon and to rule out tendon rupture. An MRI can be used for similar purposes, as well. Your physician will determine whether or not further studies are necessary.
Nonsurgical Treatment
Physical therapy is the first and most useful defense for achilles tendonitis because of the two presentations outlined above. Treatments for the two types are quite different in approach. Midsubstance tendinitis responds well to stretching, whereas insertional tendnitis tends to be aggravated more by it. Depend on your trusted physical therapist to differentiate between the two and follow their guidelines on exercises and running modifications. Running gait patterns that show excessive ?sinking postures? tend to point to the source of achilles tendon problems. Altering your gait in the midstance phase of the cycle can reduce the load on the tendon dramatically and thereby reduce pain. Rely on your running physical therapist for proper guidance on altering your gait the right way. Stride Strong?s Portland Running Clinic gait analysis can identify and fix potential issues before pain sets in. Icing at the onset of acute achilles pain (i.e. when the injury is fresh and new) would help control the inflammation. Your next step should be to call our number for an appointment.
Surgical Treatment
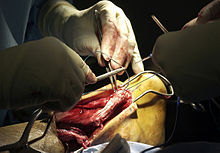
In cases of severe, long-term Achilles tendonitis the sheath may become thick and fibrous. In these cases surgery may be recommended. Surgery aims to remove the fibrous tissue and repair any tears in the tendon. A cast or splint will be required after the operation and a recovery program including physiotherapy, specific exercises and a gradual return to activity will be planned.
Prevention
Appropriately warm up and stretch before practice or competition. Allow time for adequate rest and recovery between practices and competition. Maintain appropriate conditioning, Ankle and leg flexibility, Muscle strength and endurance, Cardiovascular fitness. Use proper technique. To help prevent recurrence, taping, protective strapping, or an adhesive bandage may be recommended for several weeks after healing is complete.
 The Achilles tendon connects the calf muscles in the lower leg to the heel bone. It is the largest yet most exposed tendon in the body. Achilles tendonitis is where the Achilles tendon, and sometimes the protective sheath through which it moves, becomes inflamed, causing pain and swelling symptoms. Achilles tendonitis (also known as Achilles tendinopathy or tendonosis) is classified as an overuse injury. If left untreated it can become chronic (long-term), requiring more intensive treatment. Achilles tendonitis can also increase the risk of sustaining an Achilles tendon rupture (tear).
The Achilles tendon connects the calf muscles in the lower leg to the heel bone. It is the largest yet most exposed tendon in the body. Achilles tendonitis is where the Achilles tendon, and sometimes the protective sheath through which it moves, becomes inflamed, causing pain and swelling symptoms. Achilles tendonitis (also known as Achilles tendinopathy or tendonosis) is classified as an overuse injury. If left untreated it can become chronic (long-term), requiring more intensive treatment. Achilles tendonitis can also increase the risk of sustaining an Achilles tendon rupture (tear).
Causes
Although a specific incident of overstretching can cause an Achilles tendon disorder, these injuries typically result from a gradually progressive overload of the Achilles tendon or its attachment to bone. The cause of this chronic overload is usually a combination of factors that can put excess stress on the tendon: being overweight, having a tight calf muscle, standing or walking for a long period of time, wearing excessively stiff or flat footwear, or engaging in significant sports activity.
Symptoms
Gradual onset of pain and stiffness over the tendon, which may improve with heat or walking and worsen with strenuous activity. Tenderness of the tendon on palpation. There may also be crepitus and swelling. Pain on active movement of the ankle joint. Ultrasound or MRI may be necessary to differentiate tendonitis from a partial tendon rupture.
Diagnosis
The diagnosis is made via discussion with your doctor and physical examination. Typically, imaging studies are not needed to make the diagnosis. However, in some cases, an ultrasound is useful in looking for evidence of degenerative changes in the tendon and to rule out tendon rupture. An MRI can be used for similar purposes, as well. Your physician will determine whether or not further studies are necessary.
Nonsurgical Treatment
Physical therapy is the first and most useful defense for achilles tendonitis because of the two presentations outlined above. Treatments for the two types are quite different in approach. Midsubstance tendinitis responds well to stretching, whereas insertional tendnitis tends to be aggravated more by it. Depend on your trusted physical therapist to differentiate between the two and follow their guidelines on exercises and running modifications. Running gait patterns that show excessive ?sinking postures? tend to point to the source of achilles tendon problems. Altering your gait in the midstance phase of the cycle can reduce the load on the tendon dramatically and thereby reduce pain. Rely on your running physical therapist for proper guidance on altering your gait the right way. Stride Strong?s Portland Running Clinic gait analysis can identify and fix potential issues before pain sets in. Icing at the onset of acute achilles pain (i.e. when the injury is fresh and new) would help control the inflammation. Your next step should be to call our number for an appointment.

Surgical Treatment
In cases of severe, long-term Achilles tendonitis the sheath may become thick and fibrous. In these cases surgery may be recommended. Surgery aims to remove the fibrous tissue and repair any tears in the tendon. A cast or splint will be required after the operation and a recovery program including physiotherapy, specific exercises and a gradual return to activity will be planned.
Prevention
Appropriately warm up and stretch before practice or competition. Allow time for adequate rest and recovery between practices and competition. Maintain appropriate conditioning, Ankle and leg flexibility, Muscle strength and endurance, Cardiovascular fitness. Use proper technique. To help prevent recurrence, taping, protective strapping, or an adhesive bandage may be recommended for several weeks after healing is complete.
An Achilles Tendon Rupture How Do I Know I Suffered It?
Overview

An Achilles tendon rupture, also known as an Achilles tendon tear, is the snapping or pulling apart of the Achilles tendon into two pieces. Achilles tendon ruptures can be full ruptures or partial ruptures. A physician may be required to distinguish between acute Achilles tendinosis and a partial Achilles tendon rupture. Tennis Leg is a rupture of the connection between the calf muscle and the Achilles tendon. Achilles tendonitis is an inflammation of the Achilles tendon: it is much less common than, but often confused with, Achilles tendinosis. Achilles tendons can also be lacerated or crushed.
Causes
The tendon usually ruptures without any warning. It is most common in men between the ages of 40-50, who play sports intermittently, such as badminton and squash. There was probably some degeneration in the tendon before the rupture which may or may not have been causing symptoms.
Symptoms
Tendon strain or tendon inflammation (tendonitis) can occur from tendon injury or overuse and can lead to a rupture. Call your doctor if you have signs of minor tendon problems. Minor tenderness and possible swelling increases with activity. There is usually no specific event causing sudden pain and no obvious gap in the tendon. You can still walk or stand on your toes. Acute calf pain and swelling can indicate a tear or partial tear of the Achilles tendon where it meets the calf muscle. You may still be able to use that foot to walk, but you will need to see a specialist such as an orthopedic surgeon. Surgery is not usually done for partial tears. Sometimes special heel pads or orthotics in your shoes may help. Follow up with your doctor to check for tendonitis or strain before resuming activity, because both can increase the risk of tendon rupture. Any acute injury causing pain, swelling, and difficulty with weight-bearing activities such as standing and walking may indicate you have a tear in your Achilles tendon. Seek prompt medical attention from your doctor or emergency department. Do not delay! Early treatment results in better outcome. If you have any question or uncertainty, get it checked.
Diagnosis
Your doctor will ask you about your symptoms and examine you. He or she may also ask you about your medical history. Your doctor may ask you to do a series of movements or exercises to see how well you can move your lower leg. He or she may also examine your leg, heel and ankle and may squeeze your calf muscle to check the movement of your foot. You may need to have further tests to confirm if your tendon is torn, which may include the following. An ultrasound scan. This uses sound waves to produce an image of the inside of your leg. An MRI scan. This uses magnets and radio waves to produce images of the inside of your leg.
Non Surgical Treatment
There is no definitive protocol for conservative management. Traditionally, conservative treatment involved immobilisation in a cast or boot, with initial non-weight bearing. Recently, good results have been achieved with functional bracing and early mobilisation, and it is common to be immediately weight-bearing in an orthotic. Conservative management reduces the chance of complications, such as infection. There is a risk the tendon can heal too long and more slowly.
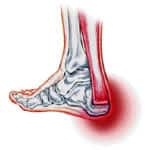
Surgical Treatment
Most published reports on surgical treatment fall into 3 different surgical approach categories that include the following: direct open, minimally invasive, and percutaneous. In multiple studies surgical treatment has demonstrated a lower rate of re-rupture compared to nonoperative treatment, but surgical treatment is associated with a higher rate of wound healing problems, infection, postoperative pain, adhesions, and nerve damage. Most commonly the direct open approach involves a 10- to 18-cm posteromedial incision. The minimally invasive approach has a 3- to 10-cm incision, and the percutaneous approach involves repairing the tendon through multiple small incisions. As with nonsurgical treatment there exists wide variation in the reported literature regarding postoperative treatment protocols. Multiple comparative studies have been published comparing different surgical approaches, repair methods, or postoperative treatment protocols.

An Achilles tendon rupture, also known as an Achilles tendon tear, is the snapping or pulling apart of the Achilles tendon into two pieces. Achilles tendon ruptures can be full ruptures or partial ruptures. A physician may be required to distinguish between acute Achilles tendinosis and a partial Achilles tendon rupture. Tennis Leg is a rupture of the connection between the calf muscle and the Achilles tendon. Achilles tendonitis is an inflammation of the Achilles tendon: it is much less common than, but often confused with, Achilles tendinosis. Achilles tendons can also be lacerated or crushed.
Causes
The tendon usually ruptures without any warning. It is most common in men between the ages of 40-50, who play sports intermittently, such as badminton and squash. There was probably some degeneration in the tendon before the rupture which may or may not have been causing symptoms.
Symptoms
Tendon strain or tendon inflammation (tendonitis) can occur from tendon injury or overuse and can lead to a rupture. Call your doctor if you have signs of minor tendon problems. Minor tenderness and possible swelling increases with activity. There is usually no specific event causing sudden pain and no obvious gap in the tendon. You can still walk or stand on your toes. Acute calf pain and swelling can indicate a tear or partial tear of the Achilles tendon where it meets the calf muscle. You may still be able to use that foot to walk, but you will need to see a specialist such as an orthopedic surgeon. Surgery is not usually done for partial tears. Sometimes special heel pads or orthotics in your shoes may help. Follow up with your doctor to check for tendonitis or strain before resuming activity, because both can increase the risk of tendon rupture. Any acute injury causing pain, swelling, and difficulty with weight-bearing activities such as standing and walking may indicate you have a tear in your Achilles tendon. Seek prompt medical attention from your doctor or emergency department. Do not delay! Early treatment results in better outcome. If you have any question or uncertainty, get it checked.
Diagnosis
Your doctor will ask you about your symptoms and examine you. He or she may also ask you about your medical history. Your doctor may ask you to do a series of movements or exercises to see how well you can move your lower leg. He or she may also examine your leg, heel and ankle and may squeeze your calf muscle to check the movement of your foot. You may need to have further tests to confirm if your tendon is torn, which may include the following. An ultrasound scan. This uses sound waves to produce an image of the inside of your leg. An MRI scan. This uses magnets and radio waves to produce images of the inside of your leg.
Non Surgical Treatment
There is no definitive protocol for conservative management. Traditionally, conservative treatment involved immobilisation in a cast or boot, with initial non-weight bearing. Recently, good results have been achieved with functional bracing and early mobilisation, and it is common to be immediately weight-bearing in an orthotic. Conservative management reduces the chance of complications, such as infection. There is a risk the tendon can heal too long and more slowly.

Surgical Treatment
Most published reports on surgical treatment fall into 3 different surgical approach categories that include the following: direct open, minimally invasive, and percutaneous. In multiple studies surgical treatment has demonstrated a lower rate of re-rupture compared to nonoperative treatment, but surgical treatment is associated with a higher rate of wound healing problems, infection, postoperative pain, adhesions, and nerve damage. Most commonly the direct open approach involves a 10- to 18-cm posteromedial incision. The minimally invasive approach has a 3- to 10-cm incision, and the percutaneous approach involves repairing the tendon through multiple small incisions. As with nonsurgical treatment there exists wide variation in the reported literature regarding postoperative treatment protocols. Multiple comparative studies have been published comparing different surgical approaches, repair methods, or postoperative treatment protocols.